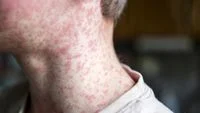
Jakarta, CNN Indonesia – The common misconception that measles is solely a childhood illness, with immunity granted for life after childhood infection or vaccination, is being challenged by medical professionals. Adults who believe they are protected may be at risk of contracting measles and facing severe complications, according to Dr. Erpryta Nurdia Tetrasiwi, an internal medicine specialist at Eka Hospital MT Haryono.
"Although measles cases are more frequently found in children, adults who do not have optimal immunity are at risk of experiencing more severe symptoms," Dr. Erpryta stated in a written statement. This elevated risk in adults stems from several key factors, primarily the natural decline of antibody levels over time and the possibility of incomplete childhood vaccination schedules.
Declining Antibody Levels and Incomplete Immunization
The immunity acquired from childhood vaccinations is not always lifelong. As individuals age, the concentration of antibodies in their system can decrease, potentially falling below the threshold required for effective protection against the virus. This gradual waning of immunity leaves adults vulnerable to infection.
Furthermore, a significant portion of the adult population may have received only a single dose of the measles vaccine in their youth. Modern research, including extensive studies conducted by the Centers for Disease Control and Prevention (CDC), has demonstrated that two doses of the Measles, Mumps, and Rubella (MMR) vaccine are necessary to achieve optimal and long-lasting protection, estimated to be around 97% effective. Individuals who received only one dose may not have built a robust enough immune defense to ward off the virus.
The highly contagious nature of the measles virus amplifies the risk. Measles can remain airborne for up to two hours after an infected person leaves a room, making public spaces such as offices, public transportation, and schools potential hotspots for transmission. This poses a significant threat to adults with compromised or insufficient immunity.
Severe Complications in Adults
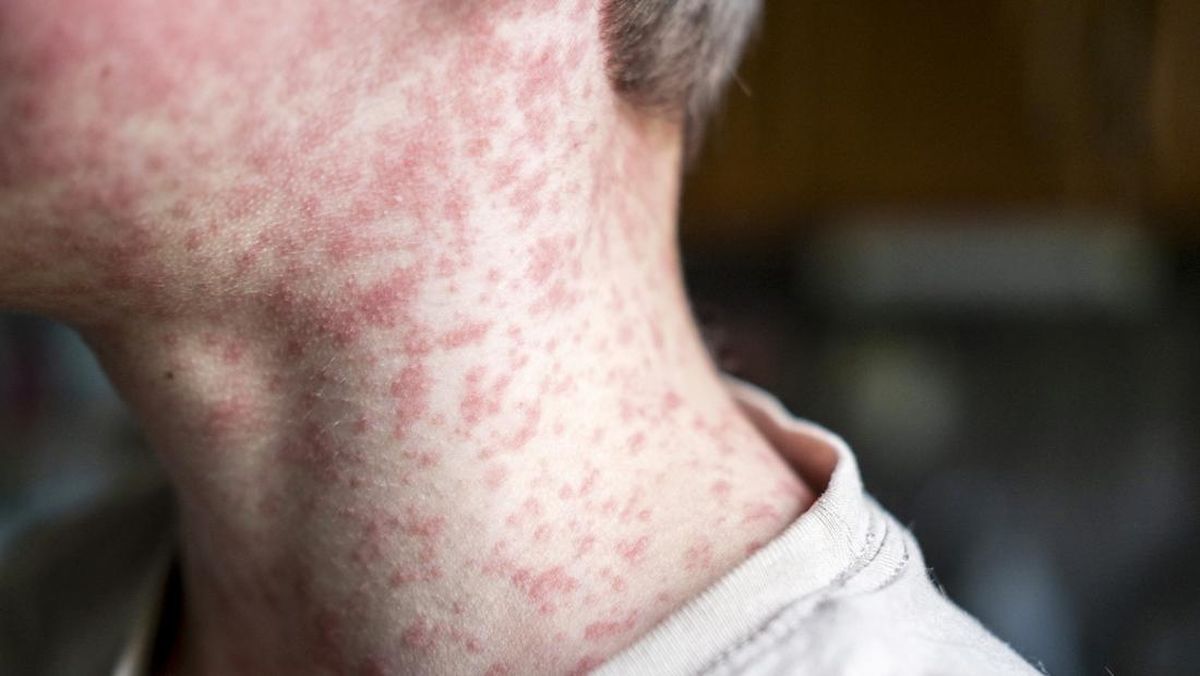
While measles in children often resolves within one to two weeks with symptoms like fever and rash, the infection can manifest more aggressively in adults. Beyond the typical symptoms, measles can profoundly weaken the entire immune system, paving the way for a cascade of serious complications.
Pneumonia: A Leading Cause of Mortality
One of the most critical and life-threatening complications of measles in adults is severe pneumonia. The measles virus can directly damage lung tissue, compromising respiratory function. Additionally, the weakened immune system becomes susceptible to secondary bacterial infections, further exacerbating the lung inflammation and increasing the risk of mortality. According to the World Health Organization (WHO), pneumonia is a leading cause of death among children with measles, and this risk is amplified in adults due to their potentially less resilient immune systems and greater susceptibility to severe disease.
Encephalitis: The Threat of Brain Inflammation
Another grave concern is encephalitis, an inflammation of the brain. Approximately one in every 1,000 adult cases of measles can progress to encephalitis. This neurological complication can lead to a range of debilitating symptoms, including seizures, hearing impairments, and in severe instances, permanent brain damage. The incidence of post-measles encephalitis in adults underscores the systemic impact of the virus beyond the respiratory tract.
Cardiac and Ocular Involvement
In rarer but still significant cases, measles can affect the heart. Myocarditis, an inflammation of the heart muscle, can occur, impairing the heart’s ability to pump blood effectively. This can lead to various cardiovascular issues, requiring immediate medical attention.
Furthermore, measles can lead to serious visual impairments. Keratitis, an inflammation of the cornea, is a potential complication that, if not promptly diagnosed and treated, can result in blindness. The virus’s ability to target multiple organ systems highlights the systemic nature of the disease.
The Role of MMR Vaccination in Adulthood
Fortunately, protection against measles can still be achieved in adulthood through vaccination. The MMR vaccine, which immunizes against measles, mumps, and rubella, serves as a crucial booster for the adult immune system. This is particularly important for several demographics:
- Individuals who never received the vaccine as children: A substantial number of adults may have missed out on childhood immunization programs for various reasons.
- Those unsure of their vaccination status: In cases where vaccination records are lost or unclear, a precautionary MMR dose is recommended.
- Women planning pregnancy: The MMR vaccine is strongly advised for women of childbearing age who are not immune to rubella, as contracting rubella during pregnancy can lead to severe birth defects. However, women are advised to wait at least one month after receiving the MMR vaccine before attempting to conceive due to the live virus components.
The CDC recommends that all individuals born after 1956 who do not have evidence of immunity should receive at least one dose of the MMR vaccine. For healthcare workers, international travelers, and those with specific risk factors, two doses may be recommended.
Broader Public Health Implications and Prevention Strategies
The resurgence of measles cases globally in recent years, often linked to declining vaccination rates, has prompted public health organizations to re-emphasize the importance of vaccination for all age groups. The potential for widespread outbreaks, particularly in densely populated areas, poses a significant challenge to healthcare systems.
Beyond vaccination, Dr. Erpryta stressed the importance of general immune system strengthening and avoiding close contact with individuals exhibiting fever and rash symptoms, especially during confirmed outbreaks. Maintaining a healthy lifestyle, including a balanced diet, adequate sleep, and regular exercise, can contribute to a robust immune response.
The implications of widespread measles in adult populations extend beyond individual health. Large-scale outbreaks can strain healthcare resources, lead to significant economic losses due to missed workdays and increased healthcare costs, and disrupt social and economic activities. Therefore, proactive vaccination campaigns and public awareness initiatives are crucial to maintaining herd immunity and preventing the resurgence of this preventable disease.
The Centers for Disease Control and Prevention (CDC) has consistently reported on the efficacy of the MMR vaccine, noting that it has been instrumental in reducing measles incidence by over 99% since its introduction in 1963. However, the gradual decline in vaccination rates in some communities has led to pockets of unvaccinated individuals, creating fertile ground for the virus to spread. For instance, outbreaks have been reported in various countries, including parts of Europe and North America, often originating in communities with lower vaccination coverage.
The ongoing efforts to combat measles are a testament to the importance of sustained public health initiatives. By understanding the risks associated with adult measles infection and actively pursuing vaccination, individuals can protect themselves and contribute to the collective immunity of their communities, safeguarding against the serious consequences of this once-common childhood disease. The message is clear: measles is not just a childhood ailment, and vigilance, coupled with timely vaccination, remains the most effective defense.







